Pharmacy Data Migration is no longer a routine technical upgrade. It is a strategic enterprise initiative that directly affects your patient safety standards, regulatory compliance posture, operational continuity, and long-term growth trajectory. If you are leading a pharmacy organization in today’s highly regulated healthcare environment, the way you approach Pharmacy Data Migration will determine whether modernization strengthens your infrastructure or exposes you to risk.
Your pharmacy systems manage prescription histories, insurance claims, refill timelines, drug interactions, controlled substance logs, reporting requirements, and audit documentation. These systems are deeply interconnected. When you upgrade platforms, consolidate locations, migrate to the cloud, or replace legacy software, every single data element must move accurately and securely. One overlooked dependency can disrupt workflows or create compliance vulnerabilities.
Pharmacy Data Migration is not simply about transferring records from one database to another. It is about protecting clinical context, preserving historical integrity, and ensuring your organization can scale confidently. If your migration strategy lacks structure, validation, and healthcare-specific oversight, you risk financial loss, audit exposure, and operational disruption.
When you approach Pharmacy Data Migration as a transformation initiative rather than a technical project, you gain more than a new system. You gain improved visibility, stronger compliance controls, better reporting capabilities, and a foundation for enterprise scalability.
This guide walks you through the strategic, operational, and technical dimensions of Pharmacy Data Migration so you can make informed decisions with confidence and clarity.
What Is Pharmacy Data Migration?
Pharmacy Data Migration is the structured process of transferring pharmacy-related data from one system to another while preserving data integrity, regulatory alignment, and workflow continuity. At its core, it ensures that the information powering your pharmacy operations remains complete, accurate, secure, and functional after a system transition.
From a technical perspective, Pharmacy Data Migration involves several coordinated steps:
- Extracting data from legacy pharmacy management systems
- Analyzing database structures and field dependencies
- Mapping legacy data fields to new system architecture
- Transforming incompatible formats or data types
- Validating data accuracy and completeness
- Securing data during transfer
- Confirming operational functionality post-migration
However, focusing only on the technical layer misses the broader picture.
From a business standpoint, Pharmacy Data Migration protects your revenue streams. It ensures insurance claims continue processing correctly, reimbursement histories remain accessible, and reporting functions support financial oversight. If billing logic fails or adjudication records are incomplete, revenue interruptions can follow quickly.
From a compliance standpoint, migration safeguards protected health information and preserves audit trails. You are responsible for maintaining adherence to HIPAA, DEA regulations, and state board requirements. Every prescription record, controlled substance entry, and access log must remain traceable and intact.
Pharmacy systems contain deeply relational data. A single prescription can connect to:
- Patient demographic profiles
- Allergy alerts
- Drug interaction databases
- Prescriber credentials
- Insurance plan details
- Inventory stock levels
- Refill authorizations
- Controlled substance classifications
If those relationships break during migration, your workflows can fail. That is why Pharmacy Data Migration demands healthcare-specific expertise. It is not generic IT data movement. It is structured healthcare data preservation.
Why Pharmacy Data Migration Is a Strategic Initiative
You may initially approach migration as a software upgrade. In reality, it touches every critical dimension of your organization.
Patient Safety Impact
Patient safety begins with data integrity. If allergy alerts do not transfer correctly or medication histories are incomplete, pharmacists may lack essential context for decision-making.
When you execute Pharmacy Data Migration correctly, you preserve:
- Complete medication histories
- Accurate refill timelines
- Reliable drug interaction alerts
- Consistent patient identification records
- Historical prescription modifications
This ensures your clinical teams maintain full visibility. It reduces the likelihood of adverse drug events caused by incomplete data. Your migration strategy directly supports patient care outcomes.
Revenue and Financial Integrity
Your pharmacy operates within a complex reimbursement environment. Claims processing depends on accurate billing codes, insurance plan mappings, copay calculations, and adjudication records.
During Pharmacy Data Migration, you must protect:
- Insurance adjudication histories
- Reimbursement adjustments
- Pricing logic structures
- Third-party billing integrations
- Financial reporting fields
If claim history data is corrupted or plan mappings are misaligned, you may face denials, delayed payments, and revenue leakage. Migration planning is, therefore, directly tied to financial stability.
Regulatory Exposure
Healthcare organizations operate under strict regulatory oversight. HIPAA requires secure handling of protected health information. DEA regulations mandate detailed controlled substance tracking. State boards require documentation retention and reporting accuracy.
According to HIPAA guidance published by the U.S. Department of Health and Human Services, organizations must implement administrative, technical, and physical safeguards to protect protected health information.
During Pharmacy Data Migration, you must ensure:
- Audit trails remain intact
- Access controls are preserved
- Controlled substance logs are complete
- Data retention timelines are maintained
- Reporting capabilities remain functional
A structured migration reduces audit risk and strengthens your compliance posture.
Types of Data Involved in Pharmacy Environments
Pharmacy Data Migration encompasses multiple data domains. Each category requires careful analysis and validation.
Clinical and Prescription Data
Clinical data forms the operational core of your pharmacy. This includes:
- Active prescriptions
- Historical prescriptions
- Dosage instructions
- Medication changes
- Refill authorizations
- Drug interaction documentation
- Allergy alerts
- Prescriber notes
Every prescription record may include timestamps, dispensing history, and insurance details. During migration, these elements must align precisely with the new system’s schema. Even small formatting differences can disrupt reporting or alert triggers.
You must verify that medication histories remain chronologically accurate and that drug interaction engines continue functioning without interruption.
Compliance and Controlled Substance Data
Controlled substance tracking is heavily regulated. Your pharmacy must maintain detailed documentation for DEA and state review.
This includes:
- Schedule classifications
- DEA numbers
- Dispensing records
- Reporting flags
- Inventory reconciliation logs
- Transaction histories
If controlled substance data is incomplete or misaligned, you risk regulatory scrutiny. During Pharmacy Data Migration, you must conduct reconciliation testing to confirm record counts and historical continuity.
Financial and Billing Data
Billing data ensures financial sustainability. This includes:
- Insurance plan details
- Claim submission histories
- Copay calculations
- Reimbursement adjustments
- Payment reconciliation logs
- Tax reporting fields
You must confirm that claim statuses remain accurate and that integration with clearinghouses continues seamlessly after migration.
Operational and Inventory Data
Inventory management supports prescription fulfillment. Migration must account for:
- Current stock levels
- Vendor relationships
- Pricing tables
- Purchase histories
- Automated reorder thresholds
- Formulary configurations
Operational logic must migrate alongside raw data. If reorder triggers or pricing rules fail, workflow efficiency suffers.
Data Integrity and Cleanliness in Enterprise Pharmacy Data Migration
Data integrity is one of the most overlooked yet most consequential elements of Pharmacy Data Migration. While organizations often focus on extraction, transfer, and validation mechanics, the underlying condition of the data itself plays a decisive role in post-migration performance.
Most pharmacy environments contain years of accumulated structural inconsistencies. Duplicate patient profiles may exist due to variations in name entry. Legacy insurance plans may remain active in the system despite being obsolete. Prescriber identifiers may appear in multiple formats. National Drug Codes (NDCs) may reflect historical substitutions or inconsistent standardization. Notes fields may contain operational workarounds created to compensate for limitations in previous systems.
When these inconsistencies are migrated without review, inefficiencies are not eliminated, they are preserved and, in some cases, amplified.
Poor data hygiene can create measurable operational friction:
- Staff must reconcile duplicate patient records at the point of service.
- Billing teams spend additional time resolving plan mapping discrepancies.
- Inventory and financial reports require manual interpretation rather than direct reliance.
- Analytics tools generate unreliable insights due to inconsistent data structures.
Clean, normalized data enhances operational predictability. It improves workflow efficiency, strengthens reporting accuracy, and supports enterprise-level decision-making. As pharmacy platforms increasingly integrate analytics engines, performance dashboards, and automation tools, structured and standardized data becomes essential. Advanced systems rely on consistent inputs. If those inputs are fragmented or poorly aligned, performance optimization is limited.
Data cleansing should therefore be viewed as a structural enhancement, not cosmetic refinement.
A disciplined Pharmacy Data Migration process incorporates formal data hygiene protocols, including:
- Duplicate patient detection and controlled record consolidation
- Insurance plan normalization and status validation
- Standardization of prescriber credentials and NDC formats
- Removal of deprecated or unused legacy fields
- Reconciliation of high-risk categories such as controlled substance records
Migration presents a rare opportunity to evaluate the full architecture of your data environment. Few operational moments provide the same level of visibility into relational dependencies, formatting inconsistencies, and legacy structural artifacts.
When Pharmacy Data Migration is approached as a data integrity reset rather than a simple transfer exercise, organizations realize measurable performance improvements immediately following go-live. Workflows become more streamlined. Reporting becomes more reliable. Compliance documentation becomes clearer. System performance becomes more predictable.
In this way, data cleanliness is not an auxiliary task within migration. It is a foundational investment in long-term operational stability and enterprise scalability.
Common Enterprise Scenarios Requiring Migration
You may encounter Pharmacy Data Migration under several enterprise circumstances.
- Replacing legacy pharmacy management systems
- Consolidating systems after mergers or acquisitions
- Integrating multi-location operations
- Migrating to cloud-based infrastructure
- Decommissioning unsupported vendors
- Implementing regulatory-driven upgrades
Each scenario introduces unique complexity. Multi-location consolidation requires normalizing inconsistent data structures. Cloud migration requires encrypted transfer protocols and network validation. Vendor decommissioning requires complete data extraction before system shutdown.
You should evaluate each migration scenario through a structured risk and dependency assessment to avoid unexpected disruptions.
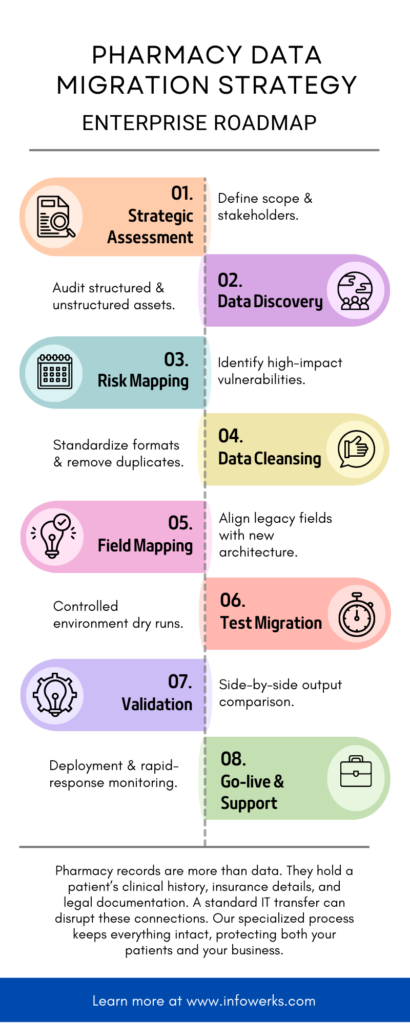
The 8-Phase Enterprise Migration Framework
A disciplined methodology reduces uncertainty and protects operational continuity. Below is a structured approach you can apply.
Phase 1: Strategic Assessment
You begin by evaluating current systems, stakeholders, compliance requirements, and operational dependencies. This phase defines scope, objectives, and measurable success criteria.
You should also identify executive sponsors and technical leads to ensure accountability throughout the migration lifecycle.
Phase 2: Data Discovery and Audit
You inventory all data assets, including structured and unstructured records. This includes identifying legacy custom fields and hidden dependencies.
You should conduct preliminary data quality analysis to detect inconsistencies before mapping begins.
Phase 3: Risk Mapping
You assess clinical, financial, and regulatory risks tied to migration. This involves identifying high-impact data elements and prioritizing validation controls.
You should document risk mitigation strategies and contingency plans for each identified vulnerability.
Phase 4: Data Cleansing
You remove duplicates, correct formatting inconsistencies, and standardize records. Data cleansing improves overall integrity before transfer.
You should implement validation checkpoints to confirm corrections do not introduce new discrepancies.
Phase 5: Field Mapping and Transformation
You align legacy data fields with the new system’s architecture. This often requires format transformation and schema normalization.
You should validate mapping logic through sample-based testing to confirm relational dependencies remain intact.
Phase 6: Test Migration
You conduct staged test migrations in controlled environments. This allows you to evaluate functionality before production deployment.
You should simulate real-world workflows to confirm system performance under operational conditions.
Phase 7: Validation and Parallel Testing
You verify data completeness, workflow functionality, and reporting accuracy. Parallel system operation allows you to compare outputs side by side.
You should conduct reconciliation reporting to confirm record counts and audit trails match expected totals.
Phase 8: Go-Live and Post-Migration Monitoring
You deploy the full migration and monitor system stability. Continuous oversight ensures rapid identification of anomalies.
You should maintain post-go-live support protocols to address issues before they escalate into operational disruptions.
Data Mapping and Validation Deep Dive
Data mapping is one of the most technically demanding aspects of Pharmacy Data Migration. You must ensure every field aligns correctly.
Field normalization requires you to confirm:
- NDC codes match standardized databases
- Prescription identifiers retain formatting structure
- Patient demographic fields align correctly
- Insurance plan codes map accurately
Validation should include:
- Record count reconciliation
- Manual audit sampling
- Automated discrepancy detection
- Cross-system comparison reports
You should combine automation tools with expert oversight to interpret anomalies accurately.
Security Architecture in Healthcare Data Migration
Healthcare data requires layered security controls. During Pharmacy Data Migration, you must implement:
- End-to-end encryption
- Secure staging environments
- Role-based access controls
- Activity logging
- Multi-factor authentication
You should also conduct penetration testing or security validation to ensure vulnerabilities are not introduced during transition.
Security cannot be an afterthought. It must be embedded into planning and execution phases.
Business Continuity and Downtime Mitigation
Pharmacies cannot tolerate prolonged downtime. You must design your migration plan around operational continuity.
Strategies include:
- Phased cutover scheduling
- Parallel system operation
- After-hours deployment windows
- Staff training before go-live
- Contingency rollback planning
You should define clear communication protocols to keep stakeholders informed throughout the process.
Technology and Automation in Modern Migration
Automation enhances efficiency and reduces manual errors. You can leverage tools for:
- Duplicate detection
- Field validation
- Data reconciliation
- Exception reporting
- Audit documentation generation
However, automation should complement human expertise. Contextual healthcare knowledge remains essential for interpreting discrepancies.
Cost Considerations and Return on Investment
Pharmacy Data Migration costs vary based on:
- Data volume
- System complexity
- Custom configurations
- Compliance requirements
- Timeline constraints
Your investment delivers measurable returns:
- Reduced compliance risk
- Improved operational efficiency
- Enhanced analytics
- Stronger cybersecurity posture
- Scalable infrastructure
Remediation after failed migration often exceeds the cost of structured implementation.
Why Specialized Healthcare IT Expertise Matters
Generic IT providers may lack pharmacy-specific insight. Pharmacy workflows involve regulatory dependencies and clinical logic that general IT teams may not fully understand.
You need expertise that understands:
- Prescription lifecycle management
- Controlled substance documentation
- Insurance adjudication processes
- Audit trail preservation
- Compliance validation
Working with a healthcare-focused partner such as Infowerks ensures your Pharmacy Data Migration is aligned with clinical, operational, and regulatory realities.
Specialized expertise transforms migration from a risky upgrade into a strategic advancement.
Frequently Asked Questions About Pharmacy Data Migration
How long does enterprise Pharmacy Data Migration take?
With most providers, enterprise Pharmacy Data Migration can take several weeks to several months depending on complexity and validation requirements. However, Infowerks performs the actual go-live cutover overnight while your pharmacy is closed, so you reopen the next business day fully operational on the new system.
How is controlled substance data validated during Pharmacy Data Migration?
Controlled substance data is validated through reconciliation testing, audit trail preservation, record count verification, and compliance checks aligned with DEA and state pharmacy regulations.
Can Pharmacy Data Migration improve system interoperability?
Yes, Pharmacy Data Migration can improve interoperability by consolidating systems, standardizing data structures, and enabling integration with modern EHR, billing, and healthcare network platforms.
What happens if data discrepancies are found after go-live?
If discrepancies appear after go-live, structured post-migration monitoring and reconciliation processes allow rapid correction while maintaining audit documentation and operational continuity.
How do you protect patient privacy during Pharmacy Data Migration?
Patient privacy is protected through encryption, role-based access controls, secure staging environments, activity logging, and strict HIPAA-aligned data handling protocols.
Is cloud-based Pharmacy Data Migration more secure than on-premise migration?
Cloud-based Pharmacy Data Migration can be just as secure as on-premise migration when implemented with proper encryption, compliance controls, access management, and enterprise-grade cybersecurity architecture.
In Conclusion: Turning Pharmacy Data Migration Into Competitive Advantage
Pharmacy Data Migration is not simply about moving data from one system to another. It is about protecting your patients, preserving your revenue, and safeguarding your compliance posture while positioning your organization for long-term scalability. Every prescription record, audit trail, insurance transaction, and controlled substance log represents both operational value and regulatory responsibility. When migration is handled strategically, you do more than upgrade software. You strengthen the foundation of your enterprise.
If you treat migration as a rushed technical conversion, you expose yourself to workflow disruptions, financial inconsistencies, and compliance risk. But when you approach Pharmacy Data Migration with structure, validation, and healthcare-specific expertise, you gain clarity, efficiency, and resilience. You create an infrastructure that supports expansion, multi-location consolidation, advanced reporting, and cloud-based innovation.
Your pharmacy ecosystem depends on reliable data relationships. When those relationships remain intact, your teams operate confidently. Your billing flows consistently. Your audits remain defensible. Your patient safety standards stay uncompromised.
Pharmacy Data Migration should empower your organization, not disrupt it. With disciplined execution, strong governance, and specialized healthcare IT guidance, you transform migration into a strategic advantage. Instead of fearing system transitions, you can leverage them to modernize operations, enhance visibility, and strengthen compliance.
When you prioritize precision and partnership, migration becomes more than a project. It becomes a catalyst for enterprise progress.
This article was reviewed by Beth Manchester, Chief Operating Officer at Infowerks Data Services, with more than 25 years of experience in independent pharmacy and healthcare data operations.

